This narrative is crucial in making a strong, memorable impression on. Because nurses spend so much time with their patients and are in a better position to observe subtle symptoms and changes in behavior, it's important that they work to develop the skills needed to produce effective nurse notes. Nursing narrative note post provides templates for writing assessment notes for recertification evaluation assessment in a home heath setting. You can attend to your patient's needs and enhan. This might include a description of a nursing visit, a specific care event, or a summary of care.
Nursing progress notes are a narrative summary of the care provided by the nurse during a patient encounter. The format used for soap notes prompts the nurse to review all evidence, including subjective and objective data and information from the assessment, before reaching a nursing diagnosis. Let's write your narrative note without blank page syndrome by using this 5 paragraph framework to guide you through the construction and the exact placement of each required section and item of your oasis nursing note. This narrative is crucial in making a strong, memorable impression on. Appropriate and legible nursing note documentation gives a precise observation of nursing assessments, condition changes, the care that was provided, and relevant patient details in sample order to support integrative medical organization to provide and deliver outstanding patient care.
Narrative notes can be tricky for nursing students…what do you write, what if you miss something, what if you muck it all up and look like a goofball? You can attend to your patient's needs and enhan. In this article, i will share 5 nursing narrative note examples + how to write them and discuss the importance of accurate charting. If there is change in pt status, another note must be written! This might include a description of a nursing visit, a specific care event, or a summary of care.
I'm looking for examples of good charting (eg discharge notes, admission notes, progress notes etc.). This might include a description of a nursing visit, a specific care event, or a summary of care. Access this nursing narrative note template to promote higher clinical outcomes and greater quality of care. The format used for soap notes prompts the nurse to review all evidence, including subjective and objective data and information from the assessment, before reaching a nursing diagnosis. Let's write your narrative note without blank page syndrome by using this 5 paragraph framework to guide you through the construction and the exact placement of each required section and item of your oasis nursing note. Because nurses spend so much time with their patients and are in a better position to observe subtle symptoms and changes in behavior, it's important that they work to develop the skills needed to produce effective nurse notes. Nurse narrative note template “on empty” ™. Nursing soap notes facilitate clinical reasoning. Nursing notes are a narrative written summary of a given nursing care encounter. Let's write your narrative note without blank page syndrome by using this 5 paragraph framework to guide you through the construction and the exact placement of each required section and item of your oasis nursing note. Craft a persuasive letter of intent: If there is change in pt status, another note must be written! It usually encloses one or two paragraphs that include the patient's care, their response to the treatment, and the interventions and education the nurse provides for the patient. In this book, i bring life to an otherwise mundane topic, provide clarity for nurses about what to say in narrative notes and how to say it, and empower nurses to feel confident that their charting tells the whole story in enough detail to defend their actions. The types of assessments performed is dependent on the facility the patient is in (inpatient versus outpatient) and on the medical diagnoses and patient complaints.
Appropriate And Legible Nursing Note Documentation Gives A Precise Observation Of Nursing Assessments, Condition Changes, The Care That Was Provided, And Relevant Patient Details In Sample Order To Support Integrative Medical Organization To Provide And Deliver Outstanding Patient Care.
Nursing progress notes are a narrative summary of the care provided by the nurse during a patient encounter. Nursing note templates and examples. Narrative nurses' notes are one of the most popular forms of nursing documentation. Not only does it protect our patients from harm, but documentation also protects our most treasured asset:
I'm Looking For Examples Of Good Charting (Eg Discharge Notes, Admission Notes, Progress Notes Etc.).
As nurses, we understand the importance of documentation. Let's write your narrative note without blank page syndrome by using this 5 paragraph framework to guide you through the construction and the exact placement of each required section and item of your oasis nursing note. Nursing progress charts include nursing progress notes and other vital information relevant to the patient’s status from admission until discharge. Never fear…i’m going to give you a quick little guide on how to write an effective, legal and appropriate narrative note.
Let's Write Your Narrative Note Without Blank Page Syndrome By Using This 5 Paragraph Framework To Guide You Through The Construction And The Exact Placement Of Each Required Section And Item Of Your Oasis Nursing Note.
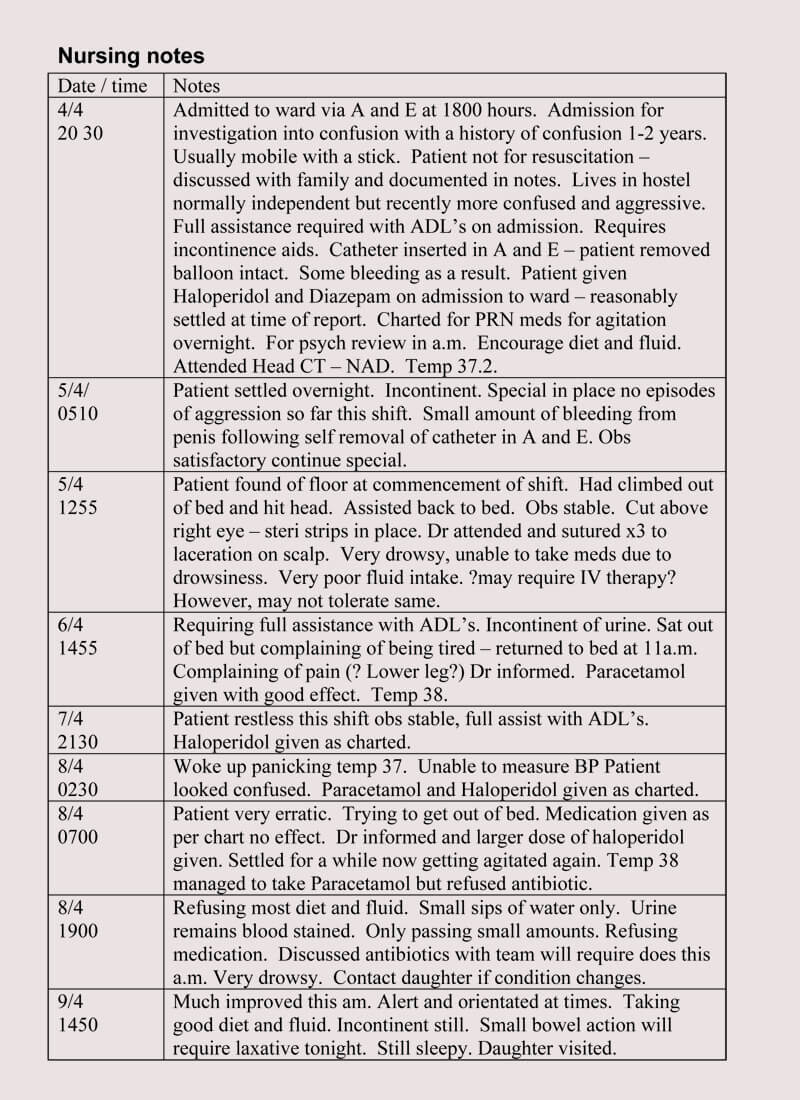
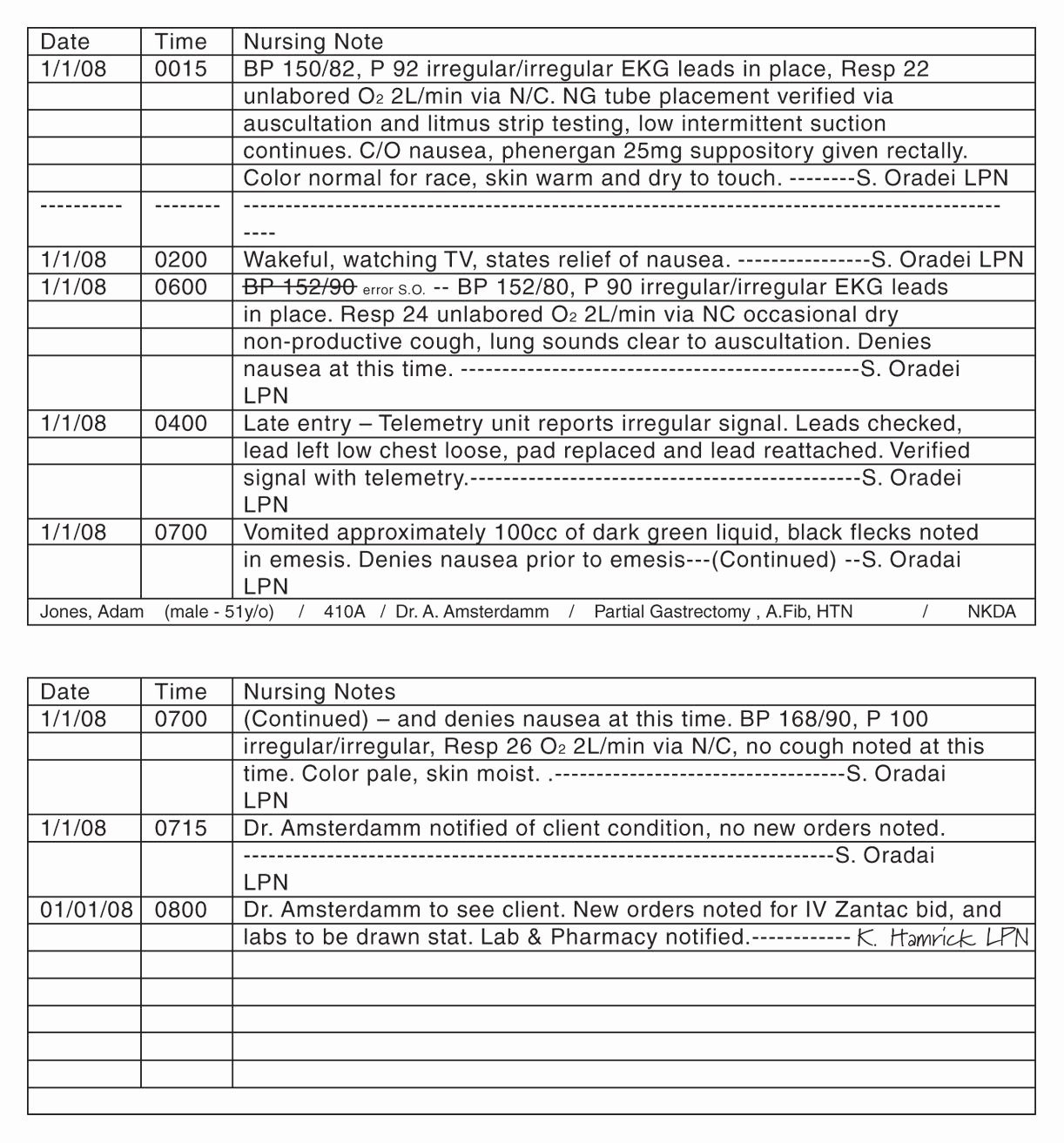
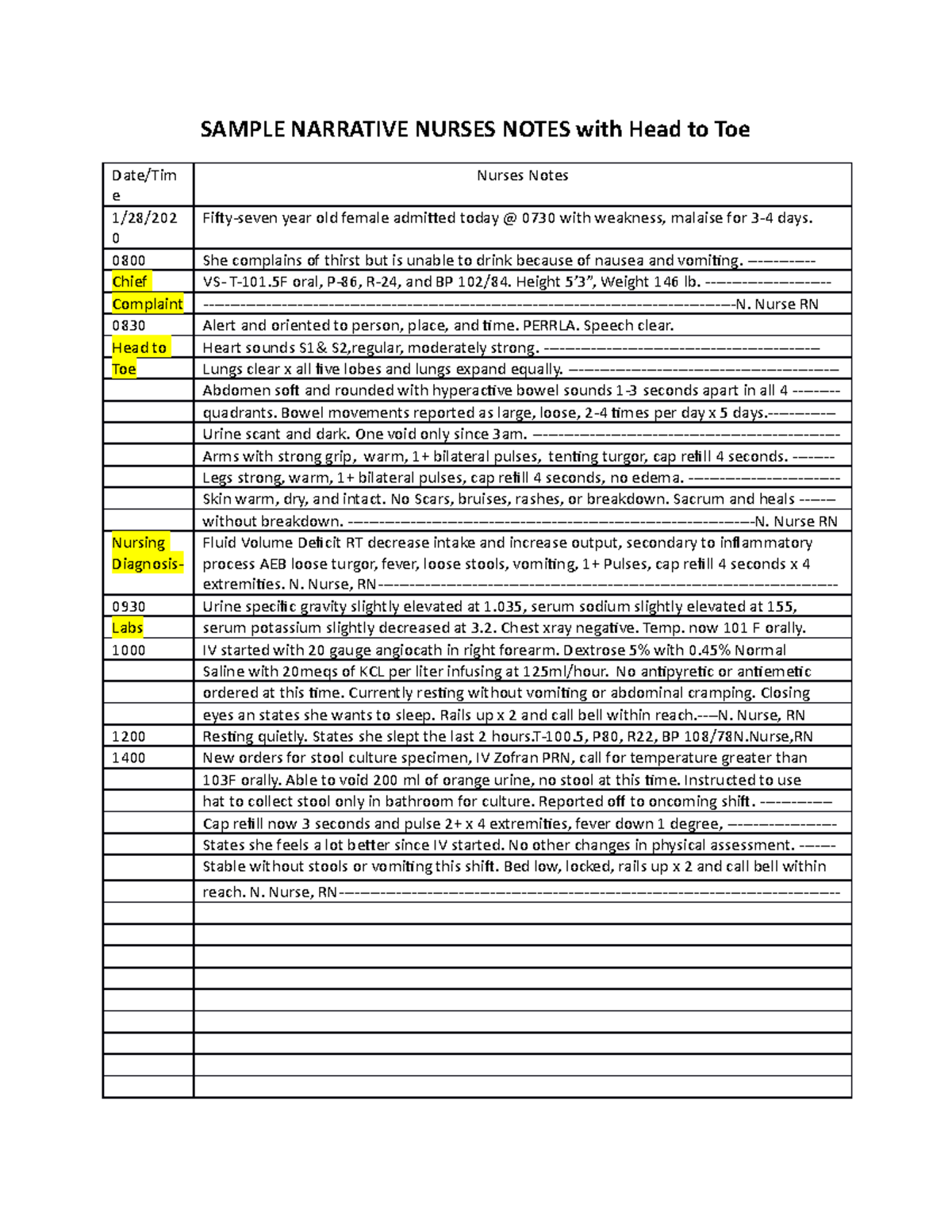
10 tips for writing effective narrative nurse's notes. Narrative notes can be tricky for nursing students…what do you write, what if you miss something, what if you muck it all up and look like a goofball? Check out our sample below for some guidance. Clinical patient narrative note (sample) one note required on each patient for your shift.
It Usually Encloses One Or Two Paragraphs That Include The Patient's Care, Their Response To The Treatment, And The Interventions And Education The Nurse Provides For The Patient.
The format used for soap notes prompts the nurse to review all evidence, including subjective and objective data and information from the assessment, before reaching a nursing diagnosis. Write a compelling letter of intent that clearly outlines your personal and professional goals, reasons for choosing nursing, and your fit for the program. The types of assessments performed is dependent on the facility the patient is in (inpatient versus outpatient) and on the medical diagnoses and patient complaints. In this book, i bring life to an otherwise mundane topic, provide clarity for nurses about what to say in narrative notes and how to say it, and empower nurses to feel confident that their charting tells the whole story in enough detail to defend their actions.



.png)