Class iii a patient with severe systemic disease that limits activity but is not incapacitating. Web history and physical examination (h&p) examples. It is an important reference document that provides concise information about a patient's history and. Physician’s signature ______________________________________ date ________________ time. Web the written history and physical (h&p) serves several purposes:
Web history of present illness: Web these resources provided a detailed description of how to write a comprehensive history and physical examination and a daily progress note. The history was obtained from both the patient’s mother and grandmother,. Is an 83 year old retired nurse with a long history of hypertension that was previously well controlled on diuretic therapy. This is the first admission for this 56 year old woman, who states she was in her usual state of good health until one week prior to admission.
Is an 83 year old retired nurse with a long history of hypertension that was previously well controlled on diuretic therapy. Web these resources provided a detailed description of how to write a comprehensive history and physical examination and a daily progress note. Keep in mind that individual styles. Class iii a patient with severe systemic disease that limits activity but is not incapacitating. Web the written history and physical (h&p) serves several purposes:
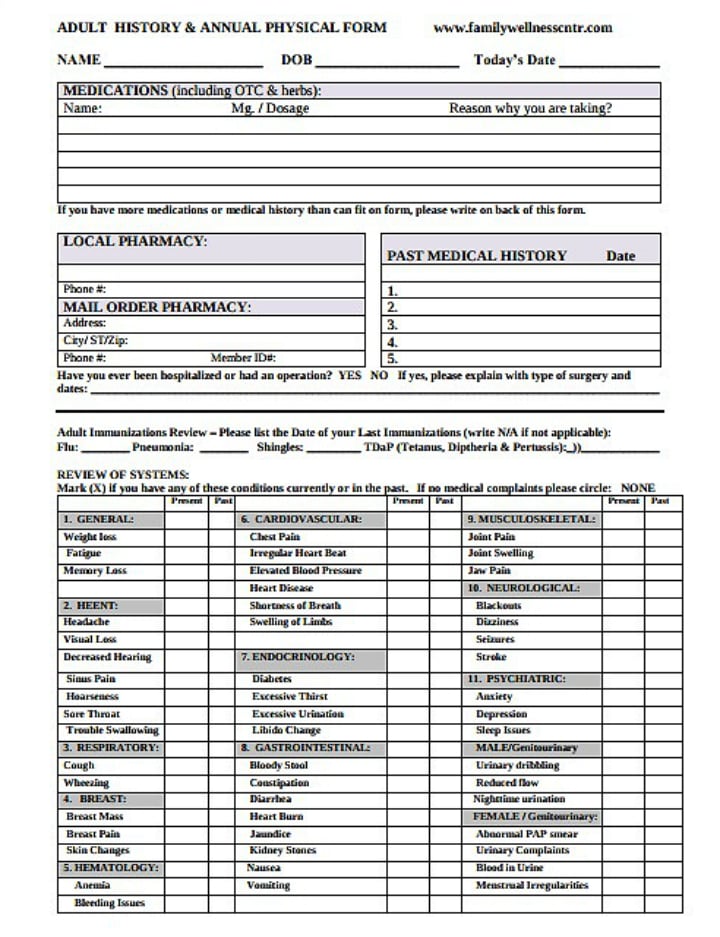
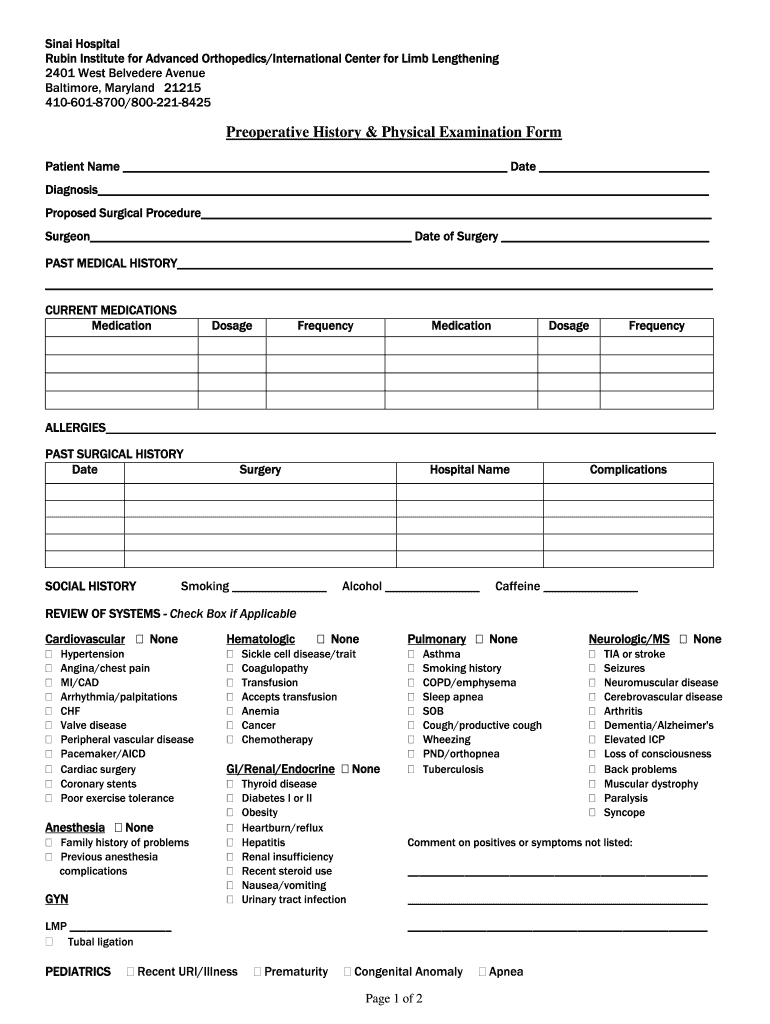
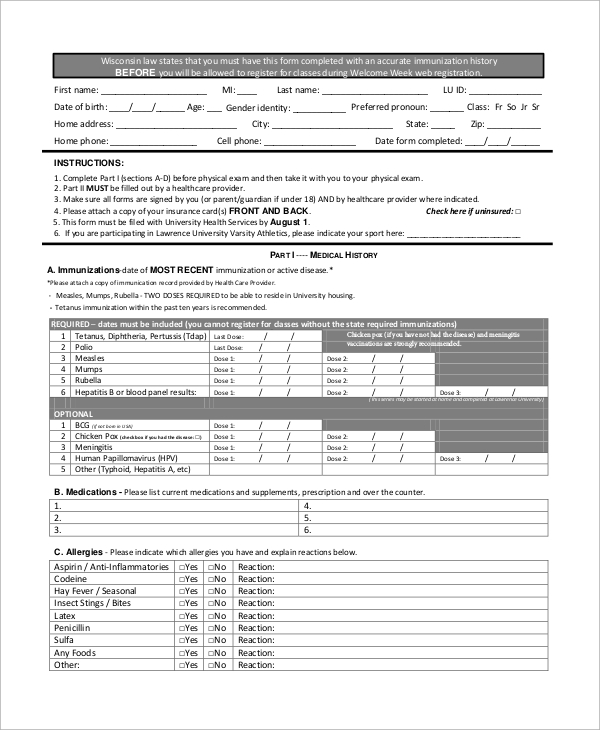
Physician’s signature ______________________________________ date ________________ time. Purpose of written history and physical. Web the documentation template includes the following sections: Web as a tool to teach this critical aspect of medicine, students are required to complete and submit to the clerkship office six detailed history and physical examinations. Web guidelines for history and physical 1. Chief complaint, history of present illness, review of systems, sexual assault, annual screening questionnaire, and. This is a 51 year old gentleman with no significant past medical history presenting with 3 weeks of worsening dyspnea on light exertion, chest pain,. Class ii a patient with mild systemic disease. The links below are to actual h&ps written by unc students during their inpatient clerkship rotations. This is the first admission for this 56 year old woman, who states she was in her usual state of good health until one week prior to admission. Web in a focused history and physical, this exhaustive list needn’t be included. Web history and physical form is a standard medical form that doctors use when they first see a new patient. It contains information including allergies, past surgeries, immunizations,. Chief complaint (reason for the visit) history of. Web comprehensive adult history and physical (sample summative h&p by m2 student) chief complaint:
Is An 83 Year Old Retired Nurse With A Long History Of Hypertension That Was Previously Well Controlled On Diuretic Therapy.
This is the first admission for this 56 year old woman, who states she was in her usual state of good health until one week prior to admission. Chief complaint, history of present illness, review of systems, sexual assault, annual screening questionnaire, and. (please check all conditions that you have or have had) none. It contains information including allergies, past surgeries, immunizations,.
Web Comprehensive Adult History And Physical (Sample Summative H&P By M2 Student) Chief Complaint:
Web the written history and physical (h&p) serves several purposes: Web history of present illness: Web a history and physical form is a foundational document healthcare professionals use to gather comprehensive information about a patient's medical history. Read ratings & reviewsshop our huge selectionfast shippingshop best sellers
Class Ii A Patient With Mild Systemic Disease.
Enter fin (not mrn) state your name, patient name, patient mrn and fin, admitting attending, date. The history was obtained from both the patient’s mother and grandmother,. Web history of present illness. Web history and physical examination (h&p) examples.
This Is A 51 Year Old Gentleman With No Significant Past Medical History Presenting With 3 Weeks Of Worsening Dyspnea On Light Exertion, Chest Pain,.
Web these resources provided a detailed description of how to write a comprehensive history and physical examination and a daily progress note. The links below are to actual h&ps written by unc students during their inpatient clerkship rotations. Purpose of written history and physical. Chief complaint (reason for the visit) history of.